[dropcap]I[/dropcap] recently spoke at a conference and one of my talks was entitled “Heart of the Matter: Cardiac Nursing”. I have delivered this talk many times before, and never had this come up. While most of the veterinary technicians and veterinarians attending the talk rated it very high, one particular comment hit home.
This talk unfortunately contained little to no cardiac nursing.
First off, I am not a speciality cardiology technician. I do not go into tremendous detail regarding things like echocardiography, 9-lead ECGs and analysis, and procedures like pacemaker placements. A cardiology technician may have a very different idea of cardiac nursing, as their focus might be different, perhaps dealing more with the diagnostics and procedures… but still nursing.
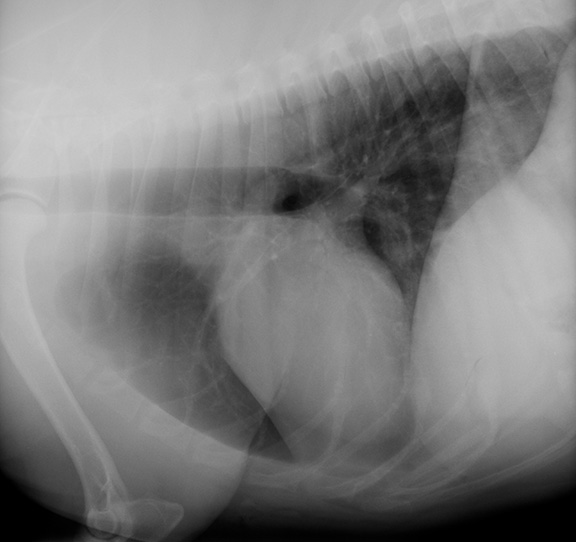
Instead, as an emergency and critical care technician, I deal primarily with the critical cardiac patient, in an ICU, requiring lots and lots of monitoring and cardiac medications. With that in mind, let me tell you what I covered in this talk. First off, I started with an overview of the anatomy and physiology of the cardiac cycle, blood flow, and conduction through the heart. I then talked about typical diagnostics that would be performed. I discussed the technique of auscultation of the heart, with a few soundbites of what might be heard over each valve and the lungs, with a few murmurs and crackles in for good measure. I went over thoracic radiographs and the importance of quality radiographs to visualize the heart, lungs and vessels. ECGs were next; a quick review on how to count off the rate on an ECG strip (yes, some monitors like to double or skip count!! 🙂 ), and review what the P, QRS, and T waves on an ECG reflect (depolarization and repolarization of specific areas of the heart). I then spent quite a bit of time on common cardiac arrhythmias, discussing the physiology of each, relating it to the conduction that we had discussed previously, and identifying the issue on ECG. Finally, we discussed echocardiography, and that this technique was generally performed by a cardiologist upon referral and showed a video of a cardiac ultrasound contrasting the ventricular contractility of a normal vs DCM heart. I discussed T-FAST ultrasound and the use in finding fluid in the pleural space, or pericardium.
I had one single slide entitled “Other Cardiac Nursing Considerations“, and I discussed the following:
- Frequent monitoring of ECG, BP, TPR and mentation
- Auscultation
- Palpation of pulses
- Identification of common arrhythmias (ECG)
- Calculation and administration of continuous rate infusions (I had an entire talk on this subject so did not go into detail)
- Pain management as necessary (also another complete talk)
I finished the talk with a few common cardiac emergencies, and discussed congestive heart failure, and why we would see pleural effusion vs ascites/venous congestion (relating back to the chambers of the heart and flow of blood through the heart and lungs that we discussed at the beginning). I talked about a couple causes of congestive heart failure we typically see. I discussed Pericardial Effusion, how a patient typically presents, findings on an ECG and auscultation, and therapeutic options that we may have to prepare for (pericardiocentesis). I touched on aortic thromboembolism, and how it may occur with HCM, and how the patient would present.
This was a one-hour talk, and obviously I could not spend a great deal of time on each topic I discussed. I realize that everything I covered cannot be expected or delivered in a general veterinary practice, but perhaps be offered at an emergency clinic or an ICU at a veterinary referral hospital. I realize as well that many of things I am talking about would not be performed by ALL veterinary technicians, however, I assume those attending the talk would have an interest. While I had only one slide called “Other Cardiac Nursing Considerations”, I strongly feel that the ENTIRE talk was on Cardiac Nursing… WHY?
As Veterinary Technicians, our job is to assist with emergencies, obtain baseline vitals including ECG and blood pressure (while ensuring accuracy of those numbers), deliver palliative options such as oxygen, pain management and/or sedation, and medications such as furosemide as ordered by our veterinarian, setup and prepare for therapeutic procedures such as a thoraco-,pericardio- or abdomino- centesis among other things. We will obtain diagnostic radiographs, perform or assist with a quick ultrasound. We may place the patient on continuous ECG, place a long-term oxygen catheter, and calculate and prepare constant rate infusion of umpteen drugs including pressors, inotropes, dilators, antiarrhythmics, antiemetics, analgesics, etc. We will also double check compatibility of each of those drugs, and recommend and place additional catheters, or a central line to deal with the compatibility. We will monitor the ECG and blood pressure, and adjust our CRIs within the dose range provided by the veterinarian, and notify them if we are approaching the high or low values of our range. We will monitor the patient’s respiratory rate and effort, and auscult the lungs if we are concerned (not just when ordered on our flowsheet). We will monitor oxygen delivery and adjust up or down as necessary (using pulse oximetry, arterial blood gases, patient demeanor and clinical signs) and notify our veterinarian of changes and need for more oxygen. We will auscult the heart and lungs, ensuring we are not hearing anything new or worsened (for example: crackles, murmurs, arrhythmias, increased or decreased heart/lung sounds).
With all of these jobs, there is a requirement for understanding. This is not only the case with cardiac nursing, but with all of the nursing that we do. We are much more effective at nursing, if we understand why we are giving the medications we are giving, understand the disease we are nursing, and understand what might happen to our patient with the disease or medications. For example, we may be given orders to increase a furosemide CRI if the patient’s respiratory rate is x. In our minds, we should be thinking… why am I increasing it?, what are we trying to achieve? what is happening within the patient??, and if we don’t know the answers, we should ask!
To be effective and well respected members of the veterinary team, it is imperative that we as veterinary technicians “up our game” and ensure that we are asserting ourselves by increasing and demonstrating our knowledge, our understanding of our patients and their conditions, recognizing concerns, and notifying our veterinarians immediately of change. We should always be asking questions, reading a book, and attending CE as much as possible to further understand what we do every day. By doing this, we increase the trust level of our veterinarians, and free them to do other things, knowing the patients are well cared for.
Perhaps I am overthinking, as I have a tendency to do… I am responding to a single comment out of about 60 attendees, and many, many more to whom I have given this exact talk. I do not know if it was a veterinary technician, or a veterinarian that wrote the comment that got me started on this post. I’m not sure which I would have preferred. In either case, I am sad that they do not feel that what I discussed is within the veterinary technician’s scope of practice, or an expectation of what a credentialed veterinary technician can and should be doing in a veterinary hospital.
All of my talks have an undercurrent of motivating veterinary technicians to seek out opportunities, better themselves by gaining knowledge, skills and certifications, and to assert themselves as valuable team members, rather than automatons who simply follow orders, and never ask a question. I feel strongly that veterinary technicians should be comfortable and encouraged to embrace this way of thinking, and if not, they should consider a move to a more progressive environment. Our profession is wrought with burnout, with potentially very good veterinary technicians leaving the profession because they do not feel valued or that they have no opportunity for professional advancement.
Consider the broader sense of “nursing”; it incorporates the critical thinking and understanding to be able to recognize when a patient is not doing well, and when a veterinarian needs to be called to the bedside. Knowledge of the condition and patient that you are nursing is vitally important to ensuring we are providing the best nursing possible.
I should mention that comments and suggestions (good and bad) following a talk are vital to how we present things in the future, and I hope that this post does not discourage anyone from speaking their mind! This comment really got me thinking, and will certainly change how I preface this talk in the future, so to the person who wrote the comment… thank you!


Leave a Reply